Wounds are also very common in daily life. With the advancement of science and technology, many methods have emerged to help wounds heal quickly. Functional medical dressings also make wounds heal faster. Up to now, medical technology has passed three major milestones. The emergence of the wound bed TIME management system has pushed wound repair technology to a new peak.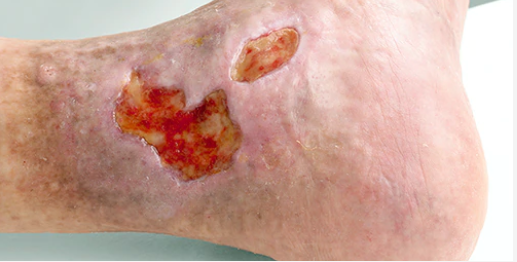
What has wound bed preparation?
Wound bed preparation is a systematic approach used by clinicians to identify and remove impediments to the wound healing process. Creating an optimal wound-healing environment through this approach focuses on (debridement, bacterial balance, and exudate management) and considers the overall health of the patient and how this may affect the wound-healing process.
What is the wound bed TIME principle?
Daily wounds can be divided into acute wounds and chronic wounds according to the healing time. For example, scalds, burns, abrasions, and scratches from sharp objects are all acute wounds. The difficulty in repairing lies in how to prevent scar hyperplasia, that is, avoid leaving scars. Bed sores, old rotten legs, chronic ulcers, diabetic feet, etc. need long-term healing and repair, which are chronic wounds. The difficulty of these wounds is to speed up the healing of the wound. Although modern medicine has reached a relatively advanced level, these two remains an important topic in the medical field. The wound bed TIME principle proposes an effective solution for both types of wounds, that is, debridement and disinfection, and antibacterial treatment are performed first, and then moist therapy is used to create an environment suitable for epithelial cell migration, so as to accelerate the acceleration of the wound and realize the docking of the epidermis. This method can transform a chronic wound into a simple wound, and then gradually shrink the wound margin until it is completely repaired.
T = Evaluation of wound tissue and management of tissue necrosis and tissue defect.
In clinical practice, one or two debridement methods are often selected and coordinated according to the conditions of the patient and the wound. For example, when the patient's physical condition is poor and surgical debridement is not suitable, conservative surgical debridement or mechanical debridement can be adopted, and then hydrogel dressing can be selected for autolytic debridement, which can not only achieve the purpose of rapid debridement but also Guarantees a complete debridement effect.
I = inflammation and infection of the wound :
Infected wounds cause patient discomfort and pain and delay the healing process. Although the focus is usually only on the bacterial burden, host resistance should be considered when determining infection risk. Malnutrition and poor tissue perfusion, smoking, substance use, comorbidities, and drug therapy reduce this resistance.
Infection treatment should start with improving host resistance by promoting healthy diets, encouraging smoking cessation, and addressing underlying conditions such as diabetes.
Interventions to control inflammation and bioburden include:
①Debridement to remove devitalized tissue
②Clean the wound with an appropriate non-cytotoxic wound cleanser
③ Use of topical antiseptics, such as dressings impregnated with antiseptics or antiseptics
④ Antibiotics are suitable for systemic infection
M = Moisture balance of the wound:
The amount of water in the wound also affects how quickly the wound bed heals, and while maintaining a moist environment is optimal for wound healing, it is a delicate balance. Excessive exudate can lead to maceration of the wound edges and tissue degradation. These damaged tissues are thought to serve as a potential source of nutrients to facilitate biofilm formation, so preventing their formation is crucial. To ensure a balanced moisture content in the wound, use a dressing that provides moisture to the wound site while absorbing excess moisture.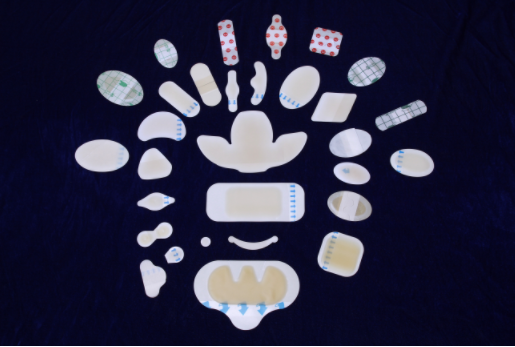
Wound care dressings that can be used for optimal moisture balance include:
①Transparent film: Helps keep the wound bed hydrated and allows gas exchange while remaining unaffected by external fluids and bacteria
②Hydrocolloid dressings: Promote autolytic debridement of dry to moderately draining wounds and help prevent infection
③Hydrogel dressings: add moisture without causing maceration to dry wounds because they are viscous water-based dressings
④ Foam dressing: used to promote healing and management of moderate to severe exudate levels in partial or full-thickness wounds
⑤Alginate Dressing: Absorb moderate to heavy exudate to achieve proper moisture balance
⑥Superabsorbent polymer: Absorbs large amounts of fluid in heavily drained wounds without drying out the wound bed
E = promotes the epithelialization process at the wound edge:
When the wound dries, epithelization and re-repair of the wound edge are retarded, and necrotic tissue and scabs develop at the wound edge.
Excessive proliferation of granulation can also affect epithelialization. Predisposing factors need to be removed (most commonly a microbiota imbalance or trauma)
Blunted or disrupted wound margins may indicate a bacterial imbalance.
For more information on Innomed® dressings, refer to the previous articles. If you have customized needs, you are welcome to contact us; we will serve you wholeheartedly.
At Longterm Medical, we transform this data by innovating and developing products that make life easier for those who need loving care.
Editor: kiki Jia
Date: November 15, 2022

 English
English عربى
عربى Español
Español русский
русский 中文简体
中文简体








