Obesity and being overweight have become major problems in society. With nearly 48 percent of African-Americans estimated to be clinically obese, obesity is known to complicate many health issues, including wound healing. How exactly does obesity affect wound healing? Below, we reveal the impact of obesity and being overweight on wound healing.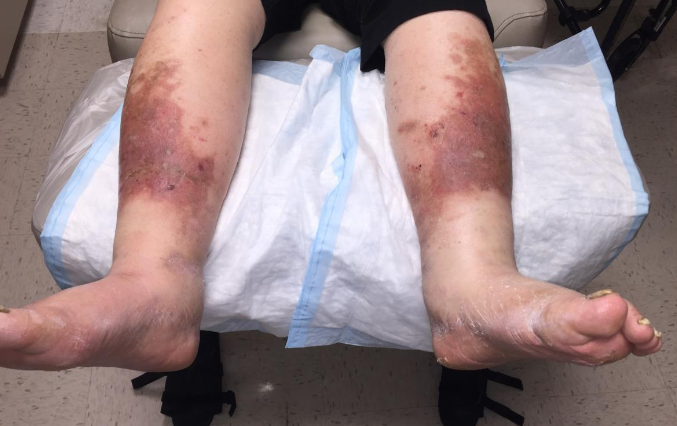
1. How to define obesity?
The World Health Organization (WHO) defines obesity as abnormal or excessive fat accumulation that poses a threat to health. It poses serious health hazards. Obesity is now considered to be a disease. At present, body mass index (BMI) is mostly used to diagnose obesity. BMI is a relatively accurate and widely accepted and adopted diagnostic method in the world. The BMI of body mass index is calculated by dividing the weight in kg by the square of the height. A body mass index greater than 25 is considered overweight, and greater than 30 is considered obese. Therefore, generally exceeding this standard can be diagnosed as obesity. In the long run, this will easily affect your health and cause other complications such as high blood pressure and high blood fat. Therefore, you must treat it correctly and correct your obesity status in time.
2. How does obesity affect wound healing?
Adipose tissue:
adipose tissue consists of thousands of cells separated by fibrous septa carrying relatively large neurons and large blood vessels. Each leaflet is supplied with blood by a vascular pedicle; the terminal capillary influx of fat lobules coupled with fewer capillary connections impedes revascularization of the graft, leading to failure, with each adipocyte surrounded by a fine capillary network. Therefore, residual fatty tissue should be removed from the lower portion of the graft before application to the donor site for maximum results.
Vascular distribution:
As adipose tissue grows, the demands placed on the circulatory system increase. As a result, adipose tissue begins to develop its own vasculature; however, capillary density does not increase with adipose tissue, so vascular insufficiency occurs. Furthermore, increased obesity leads to impaired angiogenesis and chronic low-grade inflammation. Poor blood vessels lead to poor oxygenation, which can lead to delayed normal wound healing and even tissue necrosis.
Venous insufficiency:
Vascular insufficiency is known to negatively affect wound healing as well as the development of chronic wounds. Obesity and venous insufficiency both affect wound healing, and elevated intra-abdominal pressure leads to increased reflux, increased venous diameter, increased venous pressure, and ultimately impaired venous function. Venous insufficiency causes a barrier to form around the capillaries, resulting in reduced diffusion of oxygen and other nutrients from the capillaries to surrounding tissues that need it. Due to upright pressure, intravascular fluid leaks into the interstitium surrounding the capillaries, causing an inflammatory response. Leukocytes become trapped in this fluid, causing tissue destruction due to the release of pro-inflammatory mediators and lysosomal enzymes. Taken together, obesity directly affects venous insufficiency, which in turn affects oxygenation and inflammation.
3. What challenges do pressure ulcers bring to obese patients?
Obese people are at high risk of developing pressure ulcers. Excessive weight gain predisposes to soft tissue breakdown in the bony areas that have been exposed to external pressure long enough to cause cell death.
Prolonged tissue pressure above 32 mmHg can lead to pressure necrosis. Ulcer flares present new challenges to the self-management of obese patients, often leading to non-adherence.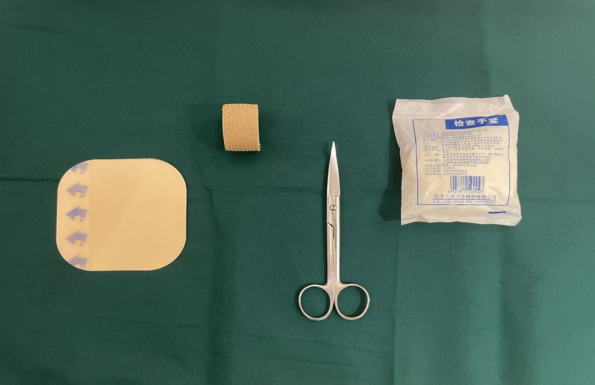
4. Wound treatment guidelines for obese patients :
When managing wounds in obese patients, caregivers must remember that they are not only treating the wound but also treating obesity-related complications. Treatment of ulcers secondary to venous insufficiency should focus on preventing infection of the ulcer.
Active infection poses a serious threat to obese people. If the ulcer is not infected, treatment should include providing an environment in which the wound can heal. Therefore, treatment can include the application of Hydrocolloid Dressing, Silver Ion Dressing, and, if there is no history of heart failure, pressure dressing. Elastic Bandage Self-Adhesive is a good option for treating ulcer patients while also fighting swelling in the lower extremities.
For more information on Innomed® elastic bandage self-adhesive, refer to the previous articles. If you have customized needs, you are welcome to contact us; we will serve you wholeheartedly.
At Longterm Medical, we transform this data by innovating and developing products that make life easier for those who need loving care.
Editor: kiki Jia
Date: December 1, 2022

 English
English عربى
عربى Español
Español русский
русский 中文简体
中文简体








