People who see alginate dressings for the first time are often surprised by its appearance—it's not the usual foam or film, but a piece that looks like white felt and feels a bit like thick non-woven fabric.
What's even more intriguing is its name. Seaweed, isn't it just that slippery stuff in the sea? How can it be made into a dressing that can stop bleeding and promote healing?
Today, I'll explain this dressing from the ocean. How exactly does it work? Why can it absorb blood while simultaneously promoting wound healing? And in what situations is it suitable for use?
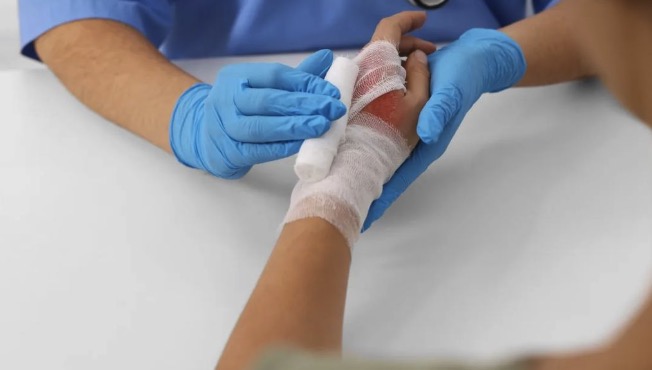
Where do alginate dressings come from?
First, let's talk about the source. The raw material for alginate dressings does indeed come from seaweed, mainly extracted from brown seaweed, such as giant kelp and sea lettuce.
Seaweed contains a substance called alginic acid, which can be processed into alginate. This alginate is then made into fibers, woven into non-woven fabric, and becomes the alginate dressing we see today.
So this stuff definitely comes from the ocean. But don't worry, after processing, it no longer looks like seaweed; instead, it's a very safe medical material. Studies have confirmed that alginate is non-toxic, non-irritating to the human body, and biodegradable.
Where does the ability to suck blood come from?
The most amazing thing about alginate dressings is that they can absorb a lot of wound exudate while also stopping bleeding.
This ability comes from a process called "ion exchange". The dressing mainly contains calcium alginate, and when it comes into contact with wound exudate (which contains sodium ions), calcium ions and sodium ions exchange.
During this exchange, the dressing fibers slowly expand, forming a soft, gel-like substance. This gel locks the exudate firmly within the fiber structure, preventing the liquid from spreading.
The result is that the dressing is fully absorbed, but the healthy skin around the wound doesn't become whitish from being soaked in exudate. This characteristic is crucial for wounds with a lot of exudate.
Studies have shown that alginate dressings can absorb up to ten times their own weight, or even more. For wounds with moderate to heavy exudation, one alginate dressing can replace several ordinary gauze dressings.
How is hemostasis achieved?
Besides absorbing fluid, hemostasis is another key function of alginate dressings.
There are two mechanisms for hemostasis. The first is the physical coagulation effect. The gel formed after the alginate fibers swell can provide a scaffold for platelets, promoting blood clot formation.
Secondly, there's a chemical aspect. Calcium ions themselves play a crucial role in the coagulation process; they are coagulation factor IV and participate in multiple coagulation steps. The calcium ions released by the dressing essentially replenish the local coagulation raw materials at the wound site.
Clinical studies have shown that wounds treated with alginate dressings bleed less than those treated with regular gauze. For minor bleeding wounds, such as those in skin graft sites or minor injuries, its hemostatic effect is very reliable.
How to promote healing?
It's already quite impressive that it can absorb and stop bleeding. But the real value of alginate dressings lies in their ability to promote healing.
There are several aspects to promoting healing.
The first is to create a moist environment. After alginate forms a gel, it provides a moist healing environment for the wound, which is the core principle of modern wound care—cells can swim and grow better in a water environment.
Secondly, there is bioactivity. Studies have found that alginate itself has certain chemotactic activity, which can promote the proliferation of fibroblasts (the cells responsible for tissue growth). At the same time, research has confirmed that alginate dressings can promote granulation tissue formation and collagen deposition, which are key steps in wound healing
Thirdly, it regulates apoptosis. Recent studies have found that alginate dressings can promote Bcl-2 expression and inhibit caspase-3 expression—both of which are related to apoptosis. Simply put, it allows living cells to thrive better and dying cells to die in a timely manner, making the healing process more orderly.
Fourthly, it allows for painless dressing changes. Once a gel forms, the dressing won't stick to newly formed granulation tissue. When changing the dressing, it can be easily rinsed off with saline solution without tearing or causing secondary bleeding. This is extremely important for chronic wounds that require frequent dressing changes.
In what situations is it suitable to use it?
The characteristics of alginate dressings determine their application.
It is best suited for wounds with moderate to heavy exudate, such as lower limb ulcers, pressure sores, and diabetic foot ulcers. These wounds often have a lot of exudate, which can be absorbed cleanly with alginate without soaking the surrounding skin.
There are also cavity-type wounds. Alginate is available in filler strips or sheets that can be inserted into wound cavities to absorb exudate and fill the space.
Postoperative care following anal fistula surgery is also one of its indications. Alginate is very suitable for wounds in special locations with excessive exudation.
When is it not appropriate to use it?
Conversely, this is not suitable in some situations.
For dry wounds or wounds with only a small amount of oozing, avoid using alginate. Its strong absorbent properties will actually draw moisture away from dry wounds, making the wound even drier and hindering healing. Hydrocolloids or hydrogels are more suitable in these cases.
For severely infected wounds, debridement and infection control are necessary first; alginate alone may not be sufficient. Sometimes it is necessary to use it in conjunction with silver ion dressings or antibacterial dressings.
How to use it for the best effect?
- Direct contact with the wound. It is used as a primary dressing, applied directly to the wound, and needs to be secured with a secondary dressing, such as gauze with tape, or covered with a foam dressing.
- It can be used moist. If the wound is dry but alginate is needed (e.g., for hemostasis), you can moisten the dressing with saline solution before applying it.
- Change dressing frequency based on exudate. Change the dressing daily if there is heavy exudate, and every two to three days if there is less exudate. In some cases, it can be used continuously for up to seven days, but this depends on the wound condition. When changing the dressing, rinse it with saline solution; the gel will dissolve, and the dressing will easily fall off.
- The packing should be applied with the right amount of tightness. When using packing to fill a wound, do not pack it too tightly; leave some room for expansion. Packing it too tightly will compress the wound and hinder healing.
For more information on Innomed®Medical Silicone Tape, refer to the Previous Articles. If you have customized needs, you are welcome to contact us; You Wholeheartedly. At longterm medical, we transform this data by Innovating and Developing Products that Make Life easier for those who need loving care.
Editor: kiki Jia

 English
English عربى
عربى Español
Español русский
русский 中文简体
中文简体








