Most people who have cared for chronic wounds have experienced that awkward moment : when a smell wafts out during dressing changes, they frown, their family covers their noses, and the patient themselves wish they could disappear into the ground.
Unpleasant odor is one of the most troublesome issues in chronic wound care. It's embarrassing and anxiety-inducing: Does this smell mean the wound is festering? Is it infected? Am I not taking good care of it?
Let's clarify this today. Where is the odor coming from? When is it a problem with the dressing? When is it an infection warning sign? And how should we deal with it?
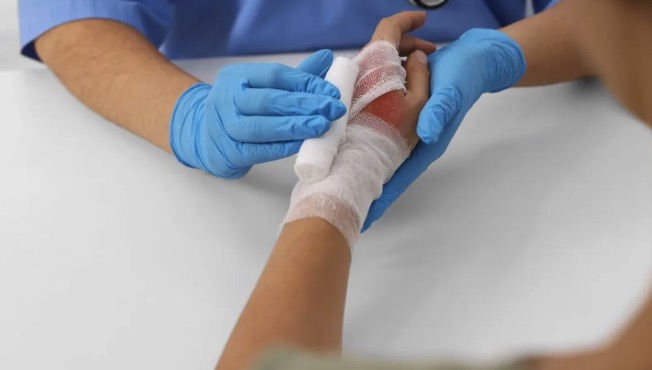
Where is the odor coming from?
Don't rush to blame yourself. An odor from a chronic wound doesn't necessarily mean you haven't taken good care of it.
There are several main sources of odor. The most common is bacterial metabolic products. Bacteria in a wound produce volatile substances during their reproduction process, such as cadaverine and putrescine. These names don't sound very pleasant, and they certainly don't smell good.
Another possibility is the decomposition of necrotic tissue. Chronic wounds often contain devitalized, non-blood-supply tissue. This tissue slowly decomposes in a moist environment, and it can also have an odor. This odor is somewhat like rotting flesh, but it is not an infection.
Another possibility is a problem with the dressing itself. Some dressings absorb exudate, and if the exudate stays inside for too long, it can react with the dressing's components, potentially producing an odor. This is usually unrelated to the wound itself; simply changing the dressing will solve the problem.
So when you smell something, the first thing to do is not to panic, but to determine the source and nature of the smell.
How can you distinguish between an infection and a dressing problem?
This is the most crucial issue. Infection and dressing problems require completely different treatments.
First, let's talk about the smell of infection. The odor caused by infection is usually strong and pungent, somewhat like rotting meat or rotten eggs. It's often accompanied by other signs: increased redness and swelling around the wound, elevated skin temperature, increased pain, cloudy or yellowish-green exudate, or fever in the patient. If even one or two of these signs are present, infection should be highly suspected.
Regarding the dressing: Odors from dressings are usually mild, slightly acidic or stuffy, and the smell disappears after changing the dressing. The wound itself looks clean, the granulation tissue is rosy, and the surrounding skin is normal; it's just that there's a slight odor when the dressing is removed. In this case, there's no need to worry too much. Just switch to a more breathable dressing or adjust the dressing change frequency.
Another simple way to tell is to observe whether the smell is coming from deep within the wound or from the surface of the dressing. Be wary if the smell is coming from deep within, and try changing the dressing if it's coming from the surface.
If it's an infection, how can dressings help?
If it's diagnosed as an infection, don't try to tough it out on your own; go to the hospital first. The doctor will need to assess the severity of the infection, which may require wound cleaning, bacterial culture, and oral or intravenous antibiotics. Dressings are supplementary at this time, not the primary treatment.
But dressings can indeed help. Choosing the right dressing while the doctor is treating the infection can help control the infection and reduce odor.
Silver ion dressings are the mainstay here. They continuously release silver ions, inhibiting bacterial growth and reducing odor-causing substances produced by bacterial metabolism. For chronic wounds that are already mildly infected or at high risk of infection, covering them with silver ion dressings is like adding an extra layer of protection.
I once saw a patient with a pressure ulcer whose wound had been there for a long time and had a strong odor. After the doctor cleaned the wound, they covered it with a silver ion dressing, changing it every three days. By the second dressing change, the odor had noticeably diminished. It wasn't that the dressing cured the infection; rather, it controlled the bacterial load, giving the body and medication time to work.
Another possibility is that the wound is infected with anaerobic bacteria, resulting in a particularly strong odor. In this case, it may be necessary to use dressings or ointments containing metronidazole, which should be used under the guidance of a doctor.
If it's not an infection, the odor might be due to the wrong dressing being chosen.
If an odor persists after ruling out infection, check if it's a problem with the dressing.
Some dressings lack absorbency, causing exudate to soak inside and inevitably develop an odor over time. In such cases, it's advisable to switch to a more absorbent dressing, such as silicone gel foam dressing. Its foam layer can absorb a large amount of exudate, locking it inside the dressing and preventing prolonged contact with the wound, thus reducing odor.
Another issue is insufficient dressing changes. When there's a lot of exudate from a chronic wound, the dressing will be saturated within a day. If you try to leave it on for two or three days, the exudate will ferment inside, inevitably producing an odor. For wounds with a lot of exudate, change the dressing daily if necessary; don't be stingy.
Another issue is the airtightness of the dressing. Some dressings are designed to be quite airtight for moisture retention. If the wound itself has an odor, the airtight environment will cause the odor to accumulate, making it particularly pungent when it's removed. In such cases, with the doctor's permission, you can appropriately increase the breathability or leave a small gap at the edge of the dressing, rather than sealing it too tightly.
If the adhesive tape used for application has a smell, or if it develops an odor after prolonged contact with skin, consider switching to silicone gel tape. It's gentle, has almost no smell, doesn't hurt when peeled off, and is friendly to the surrounding skin.
How to reduce odor in daily care?
Besides choosing the right dressing, there are some tips for daily care to reduce odor.
When changing the dressing, rinse the wound with saline solution to wash away any remaining exudate and debris. This is more effective than simply wiping it.
If permitted by your doctor, you can gently wipe around the wound with an iodine-based disinfectant to reduce surface bacteria. However, avoid poking into the wound or irritating the granulation tissue.
Used dressings should be sealed in plastic bags and thrown away immediately; do not leave them in the room. Regularly ventilate the room; the odor will dissipate with air circulation.
Another easily overlooked point is the patient's overall condition. Good blood sugar control, adequate nutrition, and a strong immune system lead to faster wound healing, lower infection risk, and naturally less odor. Chronic wounds are not a localized problem, but a systemic one.
For more information on Innomed®Silicone Foam Dressing,refer to the Previous Articles. If you have customized needs, you are welcome to contact us; You Wholeheartedly. At longterm medical, we transform this data by Innovating and Developing Products that Make Life easier for those who need loving care.
Editor: kiki Jia

 English
English عربى
عربى Español
Español русский
русский 中文简体
中文简体








