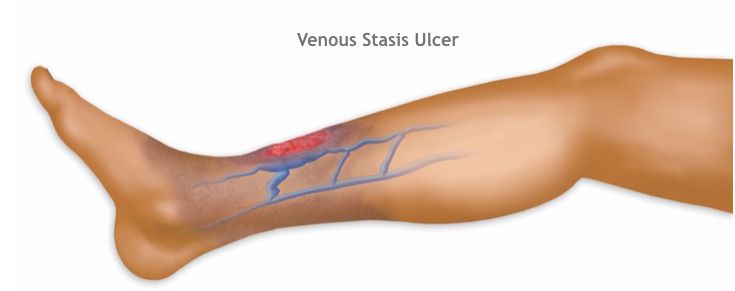
A recurring, non-healing wound on the inner side of the lower leg, surrounded by dark, hardened skin, feels cool to the touch, and is not very painful, is very likely a venous ulcer. The biggest difference between a venous ulcer and a regular injury is that its root cause is not in the wound itself, but in the venous system of the leg. Normally, when the calf muscles contract, they act like a pump, squeezing venous blood back to the heart, and the valves in the veins prevent backflow.
What exactly is the purpose of raising your leg?
The core issue of venous ulcers is the high venous pressure in the lower limbs caused by poor blood return. Elevating the leg raises it above heart level, allowing gravity to aid venous blood return. When a patient lies flat and raises their leg to about 30 degrees, the venous pressure in the lower leg drops from 80-100 mmHg when standing to near zero. Without the continuous impact of high pressure, tissue edema subsides, blood supply to the skin and subcutaneous tissue improves, and the ulcer base begins to develop healthy granulation tissue. This effect cannot be replaced by changing dressings. Dressing changes can remove exudate and necrotic tissue from the ulcer surface, creating a clean environment for healing, but if the underlying venous hypertension is not addressed, new exudate and edema will continuously flow in.
What is the correct posture and duration for leg raises?
Elevating your legs isn't as simple as just placing a pillow under your heels; there are several specific requirements. When lying down, the entire leg should be elevated above heart level, meaning from the groin, not just the foot. If only the heel is elevated, the knee will be in a drooping position, and the veins in the popliteal fossa will be blocked, affecting blood return. The correct method is to place a dedicated leg-elevating cushion or a folded blanket at the foot of the bed, providing even support from the groin to the ankle, creating a gentle incline for the entire lower limb. The back of the knee should not be unsupported, otherwise, it will cause pain over time. The elevation angle should be between 30 and 45 degrees; too high will be uncomfortable and difficult for the patient to maintain. Each leg-elevation exercise should last at least 30 minutes, accumulating to 6 to 8 hours per day. For patients who can still walk, 24-hour bed rest is not necessary. They can sit while watching TV or using their phone, placing their feet on an opposite chair or coffee table, again ensuring they are above heart level. Keep your legs elevated throughout the night while sleeping. Use a blanket or mattress to raise the foot of the bed by 10 to 15 centimeters, thus passively elevating it all night. It is important to note that if you have both arterial ischemia and venous return obstruction, consult your doctor before raising your legs, as raising your legs may worsen insufficient blood supply to the distal extremities in patients with severe arterial ischemia.
Besides leg raises, what other methods can relieve venous hypertension?
While leg elevation is effective, patients cannot lie down 24 hours a day. When standing or sitting is necessary, medical compression stockings are crucial for maintaining low venous pressure. Compression stockings apply decreasing pressure from the ankle to the thigh, with the highest pressure at the ankle and decreasing as you move upwards. This pressure gradient design mimics the action of the calf muscle pump, helping to push venous blood upwards. The choice of compression stocking pressure is important. For treating venous ulcers, the pressure typically needs to be 30 to 40 mmHg, far exceeding that of ordinary anti-varicose vein stockings. A doctor needs to measure the circumference of the ankle, calf, and thigh before prescribing them. Each morning, patients should elevate their legs for 10 to 15 minutes to reduce swelling before putting on the compression stockings. After putting them on, the pressure in the legs will be maintained at a low level. Before going to bed at night, remove the compression stockings and elevate the legs again. While wearing compression stockings, check the color of the toes. If the toes turn purple, feel cold, or feel numb, the pressure is too high, and a lower pressure level needs to be used. In addition to compression stockings, the calf muscle pump can also be strengthened through active exercise. The simplest exercise is to repeatedly flex and point your toes while sitting, doing this ten to twenty times every few minutes. This mobilizes the calf muscles to contract, squeezing venous blood back to the heart.
For more information on Innomed®Alginate Dressing, refer to the Previous Articles. If you have customized needs, you are welcome to contact us; You Wholeheartedly. At long-term medical, we transform this data by innovating and developing products that make life easier for those who need loving care.
Editor: kiki Jia

 English
English عربى
عربى Español
Español русский
русский 中文简体
中文简体








