The biggest fear when you accidentally scrape your skin, have a surgical incision, or develop a chronic leg ulcer is that it will become infected and fester. Upon seeing yellowish-white pus oozing from the wound, most people's first reaction is to use a cotton swab dipped in iodine or alcohol to vigorously wipe away the pus, then replace it with clean gauze. This approach seems reasonable—disinfection, cleaning, and bandaging—each step is correct. However, the correct order for treating infected wounds in clinical practice is exactly the opposite. It is not recommended to wipe away the pus first, and it is even more strongly discouraged to pour iodine or alcohol directly into the wound. Pus is essentially the remains of the body's immune system after fighting bacteria; it contains dead white blood cells, necrotic tissue fragments, and both living and dead bacteria. Simply wiping away the surface pus leaves bacteria and necrotic material in the deeper tissues, causing the wound to quickly re-infect. Furthermore, while iodine and alcohol can kill bacteria, they also kill newly formed cells that are actively repairing the wound, slowing healing. Modern approaches to treating infected wounds have changed. The core is not to eliminate all bacteria, but to create a controlled drainage channel while protecting the healthy tissue within the wound.
Which is safer: squeezing out pus or draining it?
Upon seeing pus, many people can't resist squeezing it out with their hands, trying to remove the pus. This action is extremely dangerous. Squeezing a wound with your hands results in dispersed and uncontrollable force, pushing pus and small plugs from the original cavity into the surrounding healthy tissue spaces, artificially expanding the infection. A small abscess cavity that was originally only one centimeter deep can, with forceful squeezing, cause pus to spur out three to five centimeters along the fascia plane. Especially in abscessed wounds in the facial triangle area, squeezing can cause pus to flow backward along the facial vein into the cavernous sinus in the brain, leading to fatal cavernous sinus thrombosis. The correct approach is not to squeeze, but to establish unobstructed drainage. If the abscess cavity is superficial, the wound edges can be gently opened with sterile forceps or tweezers to allow the pus to drain out on its own. If the abscess cavity is deep or the pus is very thick, the doctor will make a small incision at the lowest point of the abscess cavity and insert a drainage strip or tube to allow the pus to drain continuously, rather than squeezing it all out at once. The principle is similar to a clogged sink; instead of using a mop to suck up the water from the floor, you first unclog the drain and let the water drain away on its own. The drainage strip is usually left in place for two to three days, being pulled out a little each day. As the abscess cavity becomes shallower, the drainage strip gets shorter and shorter, and eventually the wound closes on its own.
How to choose dressings for a suppurating wound?
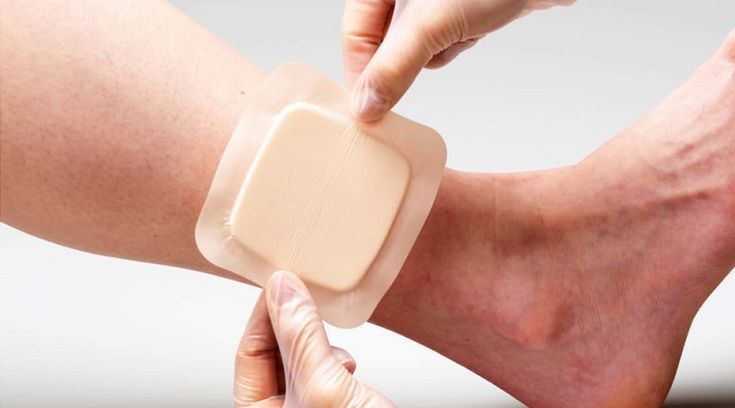
After drainage is established, wound dressing changes become a daily task. The frequency of dressing changes for suppurating wounds is higher than for ordinary wounds. For the first few days with heavy exudate, dressing changes may be needed twice a day, which can be reduced to once a day as the exudate decreases. When changing the dressing, first rinse the wound with sterile saline solution to wash away the surface pus and exudate. Saline solution is the gentlest rinsing solution and will not damage newly formed tissue. Do not use hydrogen peroxide to rinse deep wounds. Although hydrogen peroxide can kill anaerobic bacteria, the oxygen bubbles it produces can enter the interstitial spaces, worsening tissue damage and causing severe pain. After rinsing, gently absorb the moisture from the wound with sterile gauze, and then choose a dressing according to the wound's condition. If the abscess cavity is deep or the exudate is large, alginate dressings are a good choice. Alginate dressings are made from fibers extracted from brown algae. Upon contact with exudate, they turn into a soft gel that conforms to the shape of the abscess cavity, absorbing deep exudate and bacterial debris into the fibers. Alginate dressings have a mild hemostatic effect and are suitable for wounds with a small amount of bleeding from the abscess cavity. If the exudate has decreased and red granulation tissue begins to show at the base of the wound, you can switch to foam dressing or hydrocolloid dressing. These dressings have moderate absorbency, keeping the wound moist without soaking, and can be worn continuously for two to three days without changing, minimizing interference with the new granulation tissue. If the skin around the wound has become red, flaky, and itchy due to prolonged exudate irritation, you can place a ring of stoma care powder or apply a layer of zinc oxide ointment under the dressing to protect the normal skin.
For more information on Innomed® Silicone Foam Dressing, refer to the Previous Articles. If you have customized needs, you are welcome to contact us; You Wholeheartedly. At long-term medical, we transform this data by innovating and developing products that make life easier for those who need loving care.
Editor: kiki Jia

 English
English عربى
عربى Español
Español русский
русский 中文简体
中文简体








