Upon first hearing the name "Bart syndrome," many might assume it has something to do with William Harvey, the British physician who discovered blood circulation. However, this rare medical term reveals a challenge concerning the skin, blisters, and life itself from the very beginning.
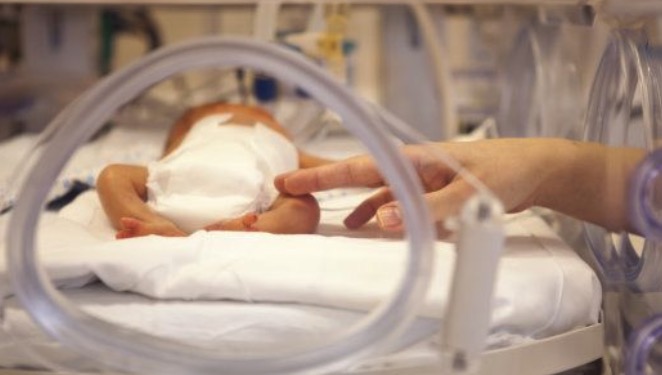
What exactly is Bart syndrome?
In simple terms, Bart syndrome is an extremely rare congenital skin disease, whose core characteristics can be summarized by three keywords: congenital skin defects, epidermolysis bullosa, and nail abnormalities.
In 1966, Dr. Bart first discovered this condition in a family—the newborn was born with a patch of skin missing from his lower leg, and subsequently developed blisters all over his body, along with nail malformation. Later, the medical community gradually clarified that this was actually a specific manifestation of epidermolysis bullosa, rather than an independent disease.
You can imagine it like this: a normal person's skin is like plywood glued together with superglue, while the skin of a child with Bart syndrome has a problem with the quality of the "glue" (type VII collagen) due to a gene mutation. The epidermis and dermis are like wallpaper that is not glued properly, and it will blister and fall off with the slightest touch.

Congenital absence
The most obvious manifestation of this disease, and the moment that most devastates parents, is that **the baby is born with a patch of skin that is "missing".**
The most common locations are the front of the lower leg and the instep, resembling a wound cut by a sharp tool, with clear borders and a base of reddish, shiny granulation tissue, possibly covered by a thin, transparent membrane. Some children have it on one side, while others have it symmetrically on both sides.
That's not all. Other areas of a baby's body prone to friction—wrists, ankles, oral mucosa, and even eyes—can also develop blisters at any time. A rub while changing a diaper or a scratch from a clothing tag can leave a new wound.
How is a diagnosis made?
While experienced dermatologists can often deduce a diagnosis from typical symptoms, a definitive diagnosis requires genetic testing. Most cases are associated with mutations in the COL7A1 gene, which encodes type VII collagen, a crucial anchor between the epidermis and dermis.
The good news is that the prognosis for Bart syndrome is relatively good. The missing skin often heals on its own with careful care, typically through epithelialization within weeks to months, eventually leaving a hypopigmented scar. The blisters may persist throughout life, but the severity varies from person to person.
Reduce the burden on delicate skin
There is currently no cure for Bart syndrome worldwide; nursing care is the entirety of treatment. The goals are simple: prevent infection, promote healing, and avoid new injury.
While reviewing case reports from both domestic and international sources, I came to a common conclusion: conservative treatment and simple methods are often the best approach.
Here I want to talk specifically about the choice of dressings. For these babies' wounds, traditional gauze is a big no-no because it will stick to the wound surface, and every time it is changed, it is an excruciating secondary injury.
This is where silicone gel foam dressings show their value. Their contact layer is a gentle silicone gel, strong enough to hold the skin in place, yet it doesn't stick to new granulation tissue when removed, maximizing protection for that thin, delicate skin. For wounds with large areas of skin loss, this painless dressing change experience not only reduces the baby's discomfort but also creates a stable environment for healing.
For fragile areas where blisters or peeling have already formed, if it's necessary to secure dressings or tubes, I would recommend using silicone gel tape. Regular tape might peel off a layer of skin when removed, while silicone gel tape is gentle enough to protect the baby's already fragile skin barrier.
If the wound shows signs of infection, the doctor may recommend using a dressing containing silver ions or an antibiotic ointment. However, in any case...
Bart syndrome, though rare, reminds us that skin is not only a barrier to the body but also a matter of life's dignity. For babies born facing the challenge of skin absence, all we can do is provide the strongest protection in the gentlest way. For more information on Innomed® Silicone Contact Layer, refer to the previous articles. If you have customized needs, you are welcome to contact us; you wholeheartedly. At long-term medical, we transform this data by innovating and developing products that make life easier for those who need loving care.
Editor: kiki Jia
( The content of this article is for general scientific information only. Please consult a professional doctor for specific treatment plans.)

 English
English عربى
عربى Español
Español русский
русский 中文简体
中文简体








